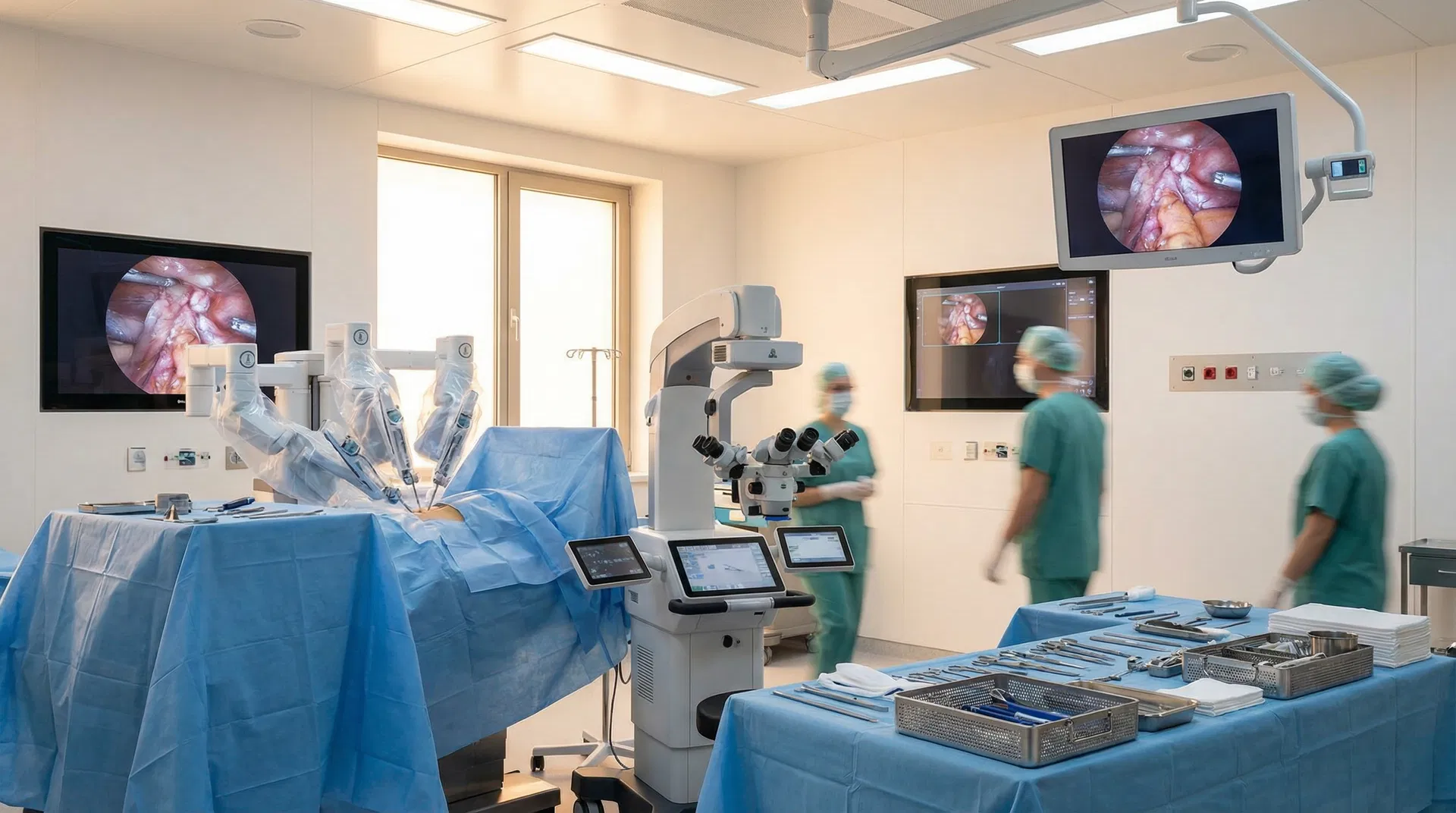
Head and Neck Tumour Surgery: From Robotic Innovation to Scarless Thyroidectomy in Hong Kong
A comprehensive guide to modern head and neck cancer surgery in Hong Kong, covering transoral robotic surgery, salvage nasopharyngectomy, scarless thyroidectomy (TOETVA), microvascular reconstruction, and sentinel lymph node biopsy — with a dedicated pathway for GCC patients.
Introduction
Head and neck cancers encompass a diverse group of malignancies arising from the oral cavity, pharynx, larynx, nasal cavity, paranasal sinuses, salivary glands, and thyroid gland. These cancers collectively represent the seventh most common cancer type worldwide, with over 900,000 new cases diagnosed annually. In Hong Kong, nasopharyngeal carcinoma (NPC) remains particularly prevalent, while thyroid cancer has seen a steady rise in incidence over the past two decades.
The management of head and neck tumours demands a uniquely multidisciplinary approach. Unlike many other cancer sites, the head and neck region houses critical structures responsible for breathing, swallowing, speech, and facial expression. Surgical intervention must therefore balance oncological radicality with functional preservation — a challenge that has driven remarkable innovations in surgical technique over the past decade.
The Multidisciplinary Team Approach
Modern head and neck cancer care is built upon the Multidisciplinary Team (MDT) model. At leading centres in Hong Kong, every cancer case is discussed and evaluated by a dedicated team comprising head and neck surgeons, plastic and reconstructive surgeons, ENT specialists, clinical oncologists, medical oncologists, radiologists, pathologists, and allied health professionals including speech therapists, dietitians, and clinical psychologists.
Regular MDT meetings ensure that each patient receives a personalised treatment plan that considers not only tumour biology and staging but also the patient's functional needs, quality of life expectations, and cultural preferences. For international patients from the Gulf Cooperation Council (GCC) countries, this holistic approach is particularly valuable, as it allows the care team to address language, dietary, and religious considerations from the outset.
Advances in Surgical Technique
Minimally Invasive and Robotic Surgery
Transoral Robotic Surgery (TORS) has emerged as a transformative approach for selected oropharyngeal and hypopharyngeal cancers. By accessing tumours through the mouth using robotic instruments, TORS eliminates the need for external incisions, reduces hospital stay, and accelerates functional recovery. Studies have demonstrated comparable oncological outcomes to open surgery with significantly lower rates of long-term swallowing dysfunction.
For parapharyngeal space tumours — traditionally requiring extensive external approaches — robotic-assisted techniques now offer a minimally invasive alternative with excellent visualisation and precise dissection around critical neurovascular structures.
Salvage Surgery for Recurrent Nasopharyngeal Carcinoma
Nasopharyngeal carcinoma presents unique surgical challenges due to the deep anatomical location of the nasopharynx and its proximity to the skull base, internal carotid arteries, and cranial nerves. When NPC recurs after primary radiotherapy, salvage nasopharyngectomy offers the only curative option for selected patients.
Hong Kong surgeons have pioneered techniques combining transnasal endoscopic and transoral robotic approaches for salvage nasopharyngectomy, achieving 5-year overall survival rates of approximately 50-65% in carefully selected patients. For locally advanced recurrences involving the skull base, craniofacial resection with extracranial-intracranial vascular bypass represents the most complex but potentially life-saving surgical option.
Thyroid Surgery: From Open to Scarless
Thyroid surgery has undergone a remarkable evolution. While conventional open thyroidectomy through a cervical collar incision remains the gold standard, the development of remote-access approaches has expanded options for patients concerned about visible neck scarring.
Transoral Endoscopic Thyroidectomy Vestibular Approach (TOETVA) represents the latest advancement in scarless thyroid surgery. By accessing the thyroid gland through three small incisions inside the lower lip, this technique leaves no visible external scar. TOETVA is suitable for selected patients with small to moderate thyroid nodules and early-stage thyroid cancers, offering equivalent oncological outcomes to open surgery with superior cosmetic results.
For patients requiring more extensive thyroid surgery, minimally invasive video-assisted thyroidectomy (MIVAT) through a 1.5-2 cm incision provides an excellent compromise between minimal scarring and surgical access.
Reconstructive Excellence
Head and neck reconstruction is integral to comprehensive cancer surgery. Modern microvascular free tissue transfer allows surgeons to reconstruct complex defects of the jaw, tongue, throat, and facial structures using tissue harvested from distant donor sites such as the forearm, thigh, or fibula.
Three-dimensional (3D) virtual surgical planning has revolutionised reconstructive accuracy. Using pre-operative CT scans, surgeons can digitally plan bone cuts, design custom reconstruction plates, and create patient-specific cutting guides. This technology reduces operative time, improves aesthetic outcomes, and enhances functional rehabilitation — particularly for patients requiring jaw reconstruction after mandibulectomy.
Sentinel Lymph Node Biopsy
For early-stage oral cavity cancers, sentinel lymph node biopsy (SLNB) offers a less invasive alternative to elective neck dissection. By identifying and removing only the first lymph nodes draining the tumour site, SLNB can accurately stage the neck while avoiding the morbidity associated with comprehensive neck dissection — including shoulder dysfunction, numbness, and lymphoedema.
International validation studies have demonstrated sensitivity rates exceeding 90% for SLNB in oral cancer, establishing it as a reliable staging tool that can spare many patients from unnecessary extensive surgery.
Skin Cancer of the Head and Neck
The head and neck region is the most common site for skin cancer due to chronic sun exposure. Surgical management requires particular expertise in achieving complete tumour excision while preserving facial aesthetics and function. Mohs micrographic surgery, combined with sophisticated local flap reconstruction, allows for precise tumour removal with maximal tissue conservation.
For advanced skin cancers requiring wider excision, microvascular free flap reconstruction provides reliable coverage with excellent functional and cosmetic outcomes.
The Patient Journey for International Patients
For GCC patients considering head and neck surgery in Hong Kong, the treatment pathway typically follows a structured approach:
- Remote Consultation: Initial case review via secure telemedicine, including evaluation of imaging studies and pathology reports.
- Arrival and Assessment: Comprehensive clinical examination, updated imaging (CT, MRI, PET-CT as indicated), and MDT discussion within 48-72 hours of arrival.
- Treatment: Surgical intervention with same-admission reconstruction when indicated, typically requiring 5-14 days of hospitalisation depending on complexity.
- Recovery: Dedicated rehabilitation with speech therapy, swallowing assessment, and nutritional support.
- Follow-up: Structured surveillance programme with telemedicine follow-up after return home, coordinated with local physicians.
Hong Kong's visa-free entry for GCC nationals, world-class hospital infrastructure, and culturally sensitive care environment make it an ideal destination for patients seeking advanced head and neck surgical treatment.
Conclusion
The field of head and neck surgery continues to evolve rapidly, driven by technological innovation and a deepening understanding of tumour biology. From robotic-assisted minimally invasive approaches to complex skull base surgery with vascular bypass, Hong Kong's head and neck surgical teams offer the full spectrum of contemporary treatment options. The integration of advanced reconstruction techniques, 3D surgical planning, and comprehensive rehabilitation ensures that patients achieve not only oncological cure but also optimal functional and aesthetic outcomes.
References
- Chan JYW, Chow VLY, Tsang R, Wei WI. Nasopharyngectomy for locally advanced recurrent nasopharyngeal carcinoma: exploring the limits. Head & Neck. 2012;34(2):229-234.
- Chan JYW, Wong STS, Chan RCL, Wei WI. Extracranial/intracranial vascular bypass and craniofacial resection: new hope for patients with locally advanced recurrent nasopharyngeal carcinoma. Head & Neck. 2016;38(S1):E2462-E2468.
- Chan JYK, Tsang R, Eisele DW, Richmon JD. Transoral robotic surgery of the parapharyngeal space: a case series and systematic review. Head & Neck. 2015;37(2):293-298.
- Lai KWK, Lai R, Lorincz BB, et al. Oncological and functional outcomes of transoral robotic surgery and endoscopic laryngopharyngeal surgery for hypopharyngeal cancer: a systematic review. Frontiers in Surgery. 2022;8:810581.
- Anuwong A, Sasanakietkul T, Jitpratoom P, et al. Transoral endoscopic thyroidectomy vestibular approach (TOETVA): indications, techniques and results. Surgical Endoscopy. 2018;32(1):456-465.
- Chow VLY, Chan JYW, Wong STW, Wei WI. Recommendations for surgical management of recurrent nasopharyngeal carcinoma. Head & Neck. 2020;42(9):2300-2307.
- Chan PLC, et al. Robotic surgery for head and neck tumors. Current Opinion in Otolaryngology & Head and Neck Surgery. 2024;32(3):156-162.
- Civantos FJ, Zitsch RP, Schuller DE, et al. Sentinel lymph node biopsy accurately stages the regional lymph nodes for T1-T2 oral squamous cell carcinomas. Journal of Clinical Oncology. 2010;28(8):1395-1400.
- Lang BH, Lo CY. Minimally invasive thyroid and parathyroid operations: surgical techniques and pearls. Advances in Surgery. 2010;44:185-198.
- Hong Kong Cancer Registry. Head and Neck Cancer Statistics 2020-2024. Hospital Authority, Hong Kong SAR.