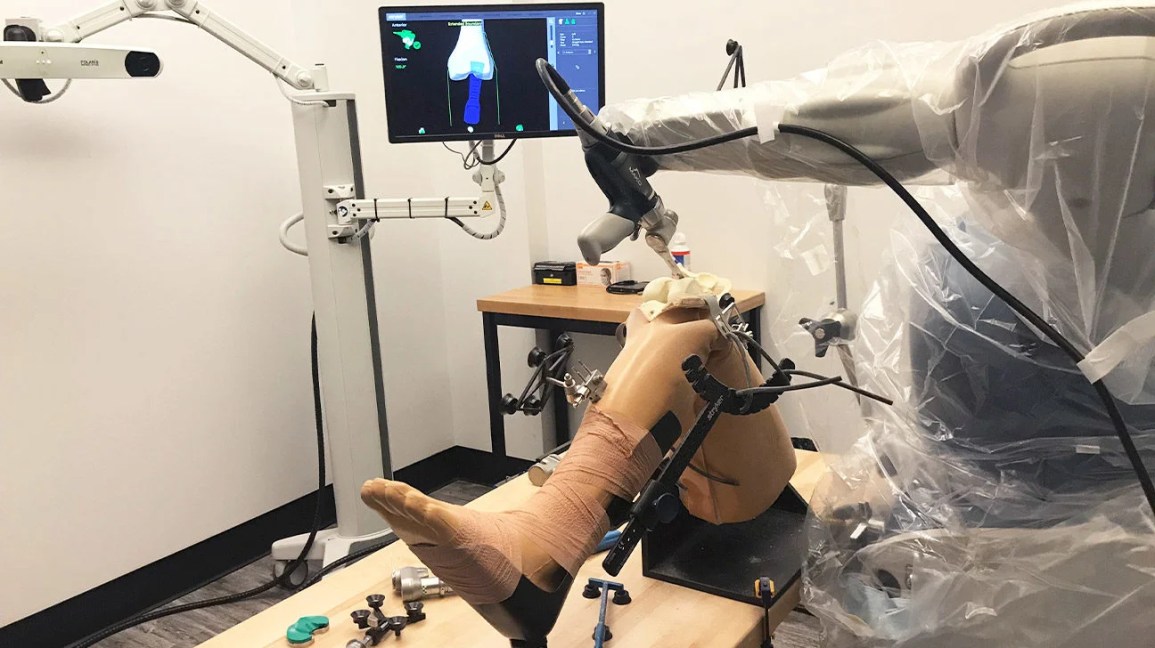
Robotic-Assisted Knee Replacement: How CT-Guided Precision Is Transforming Orthopaedic Surgery in Hong Kong
Robotic-assisted total knee arthroplasty combines CT-based 3D modelling with real-time intraoperative guidance to achieve unprecedented precision in implant positioning. Clinical evidence from 2025–2026 confirms improved alignment accuracy, faster recovery, and higher patient satisfaction compared with conventional techniques.
Introduction
Knee osteoarthritis is one of the most prevalent degenerative joint conditions worldwide, affecting an estimated 365 million people globally. In Hong Kong, the ageing population and rising obesity rates have led to a steady increase in the demand for total knee arthroplasty (TKA). For patients from the Gulf Cooperation Council (GCC) countries, where lifestyle factors and genetic predisposition contribute to high rates of knee degeneration, Hong Kong has emerged as a premier destination for advanced orthopaedic care.
The introduction of robotic-assisted total knee arthroplasty represents one of the most significant technological advances in orthopaedic surgery over the past decade. By combining CT-based three-dimensional modelling with real-time intraoperative guidance, robotic systems such as the MAKO platform enable surgeons to achieve unprecedented levels of precision in implant positioning and soft-tissue balancing.
Understanding Total Knee Arthroplasty
Total knee arthroplasty involves replacing the damaged surfaces of the knee joint with prosthetic components. The procedure addresses three compartments of the knee: the medial (inner), lateral (outer), and patellofemoral (kneecap) compartments. Success depends critically on achieving optimal implant alignment, proper ligament balance, and appropriate joint line restoration.
Traditional (conventional) TKA relies on mechanical instrumentation and the surgeon's experience to determine bone cuts and implant positioning. While this approach has a long track record of success, studies have consistently shown that 10–20% of patients remain dissatisfied with their outcomes, often due to subtle malalignment or imbalanced soft tissues that are difficult to detect intraoperatively.
How Robotic-Assisted Surgery Works
Robotic-assisted TKA follows a structured workflow that enhances each phase of the surgical process:
Preoperative Planning: A CT scan of the patient's knee is obtained and uploaded into the robotic system's software. The surgeon uses this three-dimensional model to plan the exact position, size, and orientation of each implant component. This virtual surgical plan can be adjusted to account for the patient's unique anatomy, deformity pattern, and ligament laxity.
Intraoperative Registration: During surgery, the robotic system maps the patient's actual anatomy to the preoperative CT model using optical tracking arrays attached to the femur and tibia. This registration process ensures that the virtual plan corresponds precisely to the real surgical field.
Guided Bone Preparation: The robotic arm constrains the surgeon's bone cuts to within the boundaries defined by the preoperative plan. If the saw blade deviates from the planned resection plane, the system provides haptic (tactile) feedback and can physically limit the cutting instrument's movement. This real-time guidance virtually eliminates the risk of inadvertent bone removal.
Dynamic Assessment: Throughout the procedure, the surgeon can assess ligament tension and joint kinematics in real time. The system displays gap measurements and alignment data, allowing fine adjustments to the plan before final implant placement.
Clinical Evidence: What the Research Shows
The body of evidence supporting robotic-assisted TKA has grown substantially in recent years. A 2025 systematic review and meta-analysis published in the Annals of Medicine and Surgery confirmed that robotic platforms consistently improve implant alignment accuracy and reduce outliers compared with conventional instrumentation. The study analysed data from multiple randomised controlled trials and found statistically significant improvements in both coronal and sagittal alignment.
A landmark study by Khalaf et al. (2026) demonstrated that robotic knee surgery achieved significantly better postoperative anatomical and mechanical restoration compared with conventional techniques. Similarly, research by Golinelli et al. (2025) reported that patients undergoing robotic-assisted TKA showed significant improvements in quality-of-life scores (EQ-VAS, EQ-5D-3L) and knee function scores (KOOS-PS) at six months postoperatively.
The MAKO robotic system, one of the most widely adopted platforms, has been the subject of particular scrutiny. A 2025 study published in the Bone & Joint Open found that MAKO robotic-assisted TKA was associated with improved functional outcomes. Furthermore, data from Asian public healthcare systems demonstrated that robotic TKA safely reduces hospital length of stay despite slightly longer operative times.
| Outcome Measure | Robotic-Assisted TKA | Conventional TKA |
|---|---|---|
| Implant alignment accuracy | Significantly improved | Standard |
| Alignment outliers (>3° deviation) | Reduced by 50–70% | Baseline |
| Hospital length of stay | Shorter (by 0.5–1 day) | Standard |
| 6-month quality of life (EQ-VAS) | Significantly improved | Standard |
| 5-year implant survival | >97% | >95% |
| Patient satisfaction at 1 year | Higher | Baseline |
Robotic Knee Surgery in Hong Kong
Hong Kong's adoption of robotic orthopaedic technology has been rapid and comprehensive. The University of Hong Kong (HKU) Faculty of Medicine introduced the latest robotic arm-assisted joint replacement technology to enhance surgical precision, making it available across both public and private hospital settings. Hong Kong Adventist Hospital now offers dedicated robotic-assisted knee replacement surgery packages, reflecting the growing demand from both local and international patients.
For GCC patients, Hong Kong's robotic orthopaedic capabilities offer several distinct advantages. The city's surgeons have extensive experience with the technology, having performed hundreds of robotic-assisted procedures. The multilingual healthcare environment, with Arabic interpretation services readily available, ensures clear communication throughout the treatment journey. Additionally, Hong Kong's visa-free entry policy for GCC nationals eliminates administrative barriers to accessing world-class orthopaedic care.
Who Is a Candidate for Robotic Knee Replacement?
Robotic-assisted TKA is suitable for the majority of patients who would otherwise be candidates for conventional knee replacement. Ideal candidates include individuals with moderate to severe knee osteoarthritis that has not responded adequately to conservative treatments such as physiotherapy, weight management, injections, and medication.
The technology is particularly beneficial for patients with complex deformities (significant varus or valgus malalignment), those requiring revision surgery, younger patients who demand optimal implant longevity, and individuals with high functional expectations. The precision of robotic guidance is especially valuable in these challenging cases where small differences in alignment can have outsized effects on long-term outcomes.
Recovery and Rehabilitation
Recovery following robotic-assisted TKA generally follows a similar timeline to conventional surgery, with many patients reporting faster early mobilisation due to reduced soft-tissue trauma. Most patients can bear weight on the operated leg within 24 hours of surgery and begin structured physiotherapy immediately.
A typical recovery timeline includes hospital discharge within two to three days, independent walking with aids by two weeks, return to daily activities by six weeks, and full recovery by three to six months. The precision of bone preparation in robotic surgery often translates to less postoperative pain and swelling, which can accelerate the rehabilitation process.
Conclusion
Robotic-assisted total knee arthroplasty represents a genuine paradigm shift in orthopaedic surgery. The technology's ability to deliver personalised, CT-guided surgical plans with real-time intraoperative precision has been validated by a growing body of high-quality clinical evidence. For patients seeking the highest standard of knee replacement surgery, Hong Kong's combination of advanced robotic technology, experienced surgeons, and patient-centred care makes it an outstanding destination for orthopaedic treatment.