Stereotactic Radiosurgery and Minimally Invasive Brain Tumour Surgery: Precision Neurosurgery in the Modern Era
Gamma Knife radiosurgery delivers 192 focused radiation beams with sub-millimetre precision to treat brain tumours without incision. Combined with awake craniotomy — which achieves 4.4% greater tumour resection — and intraoperative MRI, modern neurosurgery offers unprecedented precision in brain tumour treatment.
Introduction
Brain tumours represent one of the most challenging conditions in modern medicine. Whether benign or malignant, intracranial tumours demand extraordinary precision in treatment due to the brain's complexity and the critical functions of surrounding neural structures. For decades, conventional open craniotomy was the primary surgical approach, but the past two decades have witnessed a paradigm shift towards minimally invasive and non-invasive techniques that achieve comparable or superior oncological outcomes with dramatically reduced morbidity.
Stereotactic radiosurgery (SRS) and advanced minimally invasive neurosurgical techniques have emerged as transformative approaches in the management of brain tumours, vascular malformations, and functional neurological disorders. These technologies deliver treatment with millimetre-level precision, preserving healthy brain tissue while effectively targeting pathological lesions. For patients from the GCC region seeking neurosurgical care, Hong Kong's combination of world-class technology and experienced neurosurgeons makes it a premier destination for brain tumour treatment.
Stereotactic Radiosurgery: Surgery Without a Scalpel
Stereotactic radiosurgery is a non-invasive treatment that delivers a highly focused, single-session dose of radiation to a precisely defined intracranial target. Despite its name, SRS involves no surgical incision — instead, it uses multiple converging beams of radiation to create a concentrated dose at the target while minimising exposure to surrounding healthy tissue.
Gamma Knife Radiosurgery
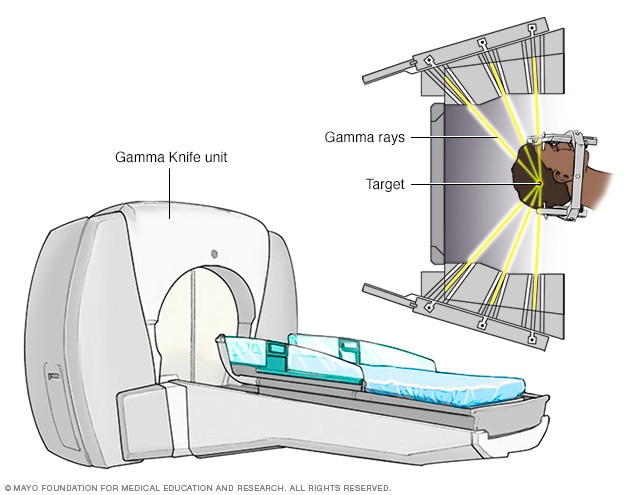
The Leksell Gamma Knife, developed by Swedish neurosurgeon Lars Leksell, remains the gold standard for intracranial stereotactic radiosurgery. The latest generation — the Gamma Knife Lightning — uses 192 precisely focused cobalt-60 radiation beams that converge on the target from multiple angles. Each individual beam carries a low dose of radiation, but at the point of convergence, the cumulative dose is sufficient to achieve the desired therapeutic effect.
The precision of Gamma Knife radiosurgery is extraordinary — treatment accuracy is typically within 0.15 mm, far exceeding the precision achievable with conventional surgical techniques. This sub-millimetre accuracy makes Gamma Knife particularly suitable for treating lesions in deep-seated or surgically inaccessible locations, including the brainstem, thalamus, and cavernous sinus.
CyberKnife Stereotactic Radiotherapy
The CyberKnife system offers an alternative approach using a robotic-mounted linear accelerator that can deliver radiation from virtually any angle. Unlike Gamma Knife, which requires a rigid head frame, CyberKnife uses real-time image guidance to track the target during treatment, allowing frameless treatment delivery. This makes CyberKnife particularly suitable for treating lesions in the spine and other extracranial locations, as well as for hypofractionated treatment schedules that deliver the radiation dose over multiple sessions.
Clinical Applications and Outcomes
| Indication | Treatment Modality | Typical Dose | Expected Outcome |
|---|---|---|---|
| Brain metastases (1–4 lesions) | Gamma Knife / CyberKnife | 18–24 Gy single fraction | Local control >85% at 1 year |
| Vestibular schwannoma | Gamma Knife | 12–13 Gy | Tumour control >95% at 10 years |
| Meningioma (small/medium) | Gamma Knife / CyberKnife | 12–16 Gy | Tumour control >90% at 10 years |
| Arteriovenous malformation | Gamma Knife | 16–25 Gy | Obliteration 70–80% at 3 years |
| Trigeminal neuralgia | Gamma Knife | 80–90 Gy to nerve root | Pain relief >80% at 1 year |
| Pituitary adenoma (residual) | Gamma Knife | 12–16 Gy | Tumour control >90% at 10 years |
Awake Craniotomy: Precision Through Patient Participation
For brain tumours located in or near eloquent cortical regions — areas responsible for speech, motor function, sensation, and vision — awake craniotomy has emerged as a powerful technique that maximises tumour resection while preserving neurological function.
During awake craniotomy, the patient is sedated for the initial stages of surgery (skull opening) but is awakened during the critical phase of tumour removal. While the neurosurgeon carefully resects the tumour, the patient performs specific tasks — speaking, moving limbs, identifying objects — that allow real-time monitoring of neurological function. If the surgeon approaches a critical functional boundary, the patient's performance on these tasks provides immediate feedback, allowing the surgeon to adjust the resection strategy.
A comprehensive meta-analysis published in 2026 by Nowacka and colleagues demonstrated that awake craniotomy achieves a greater extent of resection compared with surgery under general anaesthesia, with a mean difference of 4.4% in extent of resection. The study also found notably shorter hospital stays following awake craniotomy. For tumours in eloquent areas, this technique offers the optimal balance between maximising tumour removal and preserving the patient's quality of life.
Advanced Intraoperative Technologies
Modern neurosurgery integrates multiple advanced technologies to enhance surgical precision and safety.
Intraoperative MRI (iMRI): Real-time MRI scanning during surgery allows the neurosurgeon to visualise residual tumour that may not be apparent to the naked eye. Studies published in 2025 have demonstrated that virtual iMRI in combination with intraoperative imaging represents a promising advance in brain tumour surgery, enabling more complete resections.
Fluorescence-Guided Surgery (5-ALA): The fluorescent agent 5-aminolevulinic acid (5-ALA) is administered orally before surgery. Tumour cells selectively metabolise 5-ALA to produce a fluorescent compound (protoporphyrin IX) that glows pink-violet under blue light. This fluorescence helps the surgeon distinguish tumour tissue from normal brain, facilitating more complete resection of high-grade gliomas.
Neuronavigation: Computer-assisted surgical navigation systems integrate preoperative MRI and CT data to provide real-time three-dimensional guidance during surgery. The neurosurgeon can track the position of surgical instruments relative to the tumour and critical brain structures, enhancing precision and safety.
Intraoperative Neurophysiological Monitoring: Continuous monitoring of motor evoked potentials (MEPs), somatosensory evoked potentials (SSEPs), and electromyography (EMG) during surgery provides real-time feedback on the functional integrity of neural pathways, alerting the surgical team to potential injury before it becomes irreversible.
Neurosurgery in Hong Kong: World-Class Expertise
Hong Kong's neurosurgical services are among the most advanced in Asia. The city's neurosurgeons are fellowship-trained at leading international centres and maintain active involvement in clinical research and technological innovation. Major neurosurgical centres in Hong Kong are equipped with Gamma Knife and CyberKnife systems, intraoperative MRI suites, neuronavigation platforms, and comprehensive neurophysiological monitoring capabilities.
The Brain Centre in Hong Kong operates the Leksell Gamma Knife Lightning, one of the most advanced radiosurgery platforms in the world. This facility has treated thousands of patients with brain tumours, vascular malformations, and functional disorders, achieving outcomes that compare favourably with leading international centres.
For GCC patients, Hong Kong's neurosurgical services offer several compelling advantages. The concentration of advanced technology and experienced specialists in a compact, accessible city means that patients can receive comprehensive evaluation and treatment without the logistical challenges of navigating a large healthcare system. The availability of Arabic interpretation services ensures clear communication during what is often an anxiety-provoking treatment journey.
Who Is a Candidate for These Treatments?
The choice between stereotactic radiosurgery and microsurgical resection depends on multiple factors, including tumour type, size, location, the patient's neurological status, and overall health. In many cases, these approaches are complementary rather than competing — for example, a patient may undergo surgical resection of the main tumour mass followed by radiosurgery to treat residual or recurrent disease.
Stereotactic radiosurgery is particularly suitable for small to medium-sized tumours (typically less than 3 cm in diameter), tumours in deep or surgically inaccessible locations, patients who are not candidates for open surgery due to medical comorbidities, recurrent tumours after prior surgery, and multiple brain metastases.
Microsurgical resection with advanced intraoperative technologies is preferred for larger tumours causing mass effect, tumours requiring tissue diagnosis, tumours in accessible locations where complete resection is achievable, and cases where immediate decompression of neural structures is needed.
Conclusion
The convergence of stereotactic radiosurgery, awake craniotomy, and advanced intraoperative technologies has transformed brain tumour treatment from a field defined by the limitations of conventional surgery to one where precision, personalisation, and preservation of function are paramount. Hong Kong's neurosurgical centres, equipped with the latest Gamma Knife and CyberKnife systems, intraoperative MRI, and fluorescence-guided surgery capabilities, offer patients from the GCC region access to the full spectrum of modern neurosurgical care in a supportive, multilingual environment.