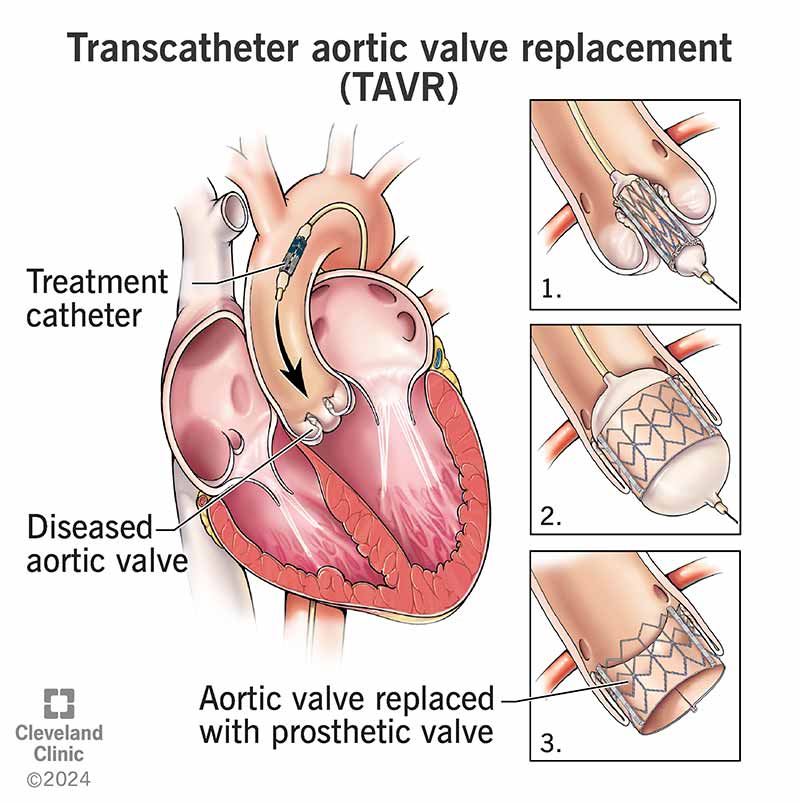
Transcatheter Aortic Valve Implantation (TAVI): How Catheter-Based Technology Is Revolutionising the Treatment of Aortic Stenosis
Transcatheter aortic valve implantation (TAVI) has transformed the treatment of severe aortic stenosis from major open-heart surgery to a minimally invasive, catheter-based procedure. Five-year and six-year data from the PARTNER 3 and Evolut Low Risk trials confirm comparable outcomes to surgery across all risk categories, with dramatically faster recovery.
Introduction
Aortic stenosis (AS) is the most common valvular heart disease in the developed world, affecting approximately 3–5% of adults over the age of 75. As the global population ages, the prevalence of degenerative aortic stenosis continues to rise, creating an urgent need for effective treatment options. For decades, surgical aortic valve replacement (SAVR) was the only definitive treatment, but the introduction of transcatheter aortic valve implantation (TAVI) — also known as transcatheter aortic valve replacement (TAVR) — has fundamentally transformed the management of this condition.
TAVI involves the deployment of a bioprosthetic valve through a catheter, typically inserted via the femoral artery, without the need for open-heart surgery or cardiopulmonary bypass. Since the first-in-human procedure performed by Dr. Alain Cribier in 2002, TAVI has evolved from a last-resort option for inoperable patients to a mainstream treatment for patients across the entire surgical risk spectrum.
The Evolution of Evidence: From High-Risk to Low-Risk Patients
The evidence base supporting TAVI has expanded dramatically through a series of landmark randomised controlled trials. The PARTNER and Evolut trial programmes have systematically demonstrated the safety and efficacy of TAVI across progressively lower-risk patient populations.
The most recent milestone came with the publication of five-year and six-year follow-up data from these pivotal trials. The PARTNER 3 trial, published in the New England Journal of Medicine in 2025, reported that five-year outcomes of TAVR versus surgery in low-risk patients showed similar clinical outcomes and valve durability. The composite endpoint of death, stroke, or rehospitalisation was comparable between the two approaches.
The Evolut Low Risk trial six-year results, presented at the American College of Cardiology Scientific Sessions in March 2026, confirmed no significant differences in death or adverse outcomes between transcatheter and surgical approaches. These findings provide compelling evidence that TAVI is a viable alternative to surgery even for younger, healthier patients with severe aortic stenosis.
| Trial | Follow-up | Population | Key Finding |
|---|---|---|---|
| PARTNER 3 | 5 years | Low surgical risk | Similar all-cause mortality and stroke rates |
| PARTNER 3 | 7 years | Low surgical risk | All-cause death: TAVR 19.5% vs SAVR 16.8% |
| Evolut Low Risk | 5 years | Low surgical risk | Comparable mortality and disabling stroke |
| Evolut Low Risk | 6 years | Low surgical risk | No significant differences in death or adverse outcomes |
| UK TAVI | 5 years | All-comers | Non-inferior to surgery |
| NOTION-2 | 5 years | Low-intermediate risk | Similar outcomes |
How TAVI Works: The Procedure Explained
The TAVI procedure represents a remarkable feat of cardiovascular engineering. The most common approach — transfemoral TAVI — is performed through a small puncture in the femoral artery in the groin, requiring no chest incision and no general anaesthesia in many cases.
Pre-procedural Planning: Cardiac CT angiography provides detailed three-dimensional imaging of the aortic root, allowing precise measurement of the aortic annulus and selection of the optimal valve size. This personalised planning is critical to achieving an optimal seal and minimising complications such as paravalvular leak.
Valve Deployment: The replacement valve, crimped onto a delivery catheter, is advanced through the arterial system to the diseased aortic valve. Under fluoroscopic and echocardiographic guidance, the new valve is deployed within the calcified native valve. Modern self-expanding and balloon-expandable valve designs allow precise positioning with the ability to recapture and reposition if needed.
Immediate Assessment: Following deployment, haemodynamic measurements and echocardiography confirm proper valve function, including assessment of any paravalvular regurgitation. Most patients experience immediate haemodynamic improvement.
Recovery: Unlike open-heart surgery, which typically requires a sternotomy, cardiopulmonary bypass, and a recovery period of six to eight weeks, TAVI patients are often mobilised within hours of the procedure. Hospital discharge within 24–48 hours is increasingly common, and many patients return to normal activities within one to two weeks.
TAVI in Hong Kong: A Regional Centre of Excellence
Hong Kong has established itself as a leading centre for structural heart intervention in Asia. The city's major cardiac centres — including Queen Mary Hospital, Prince of Wales Hospital, and several private institutions — have extensive experience with TAVI, having performed hundreds of procedures using both self-expanding and balloon-expandable valve platforms.
The Chinese University of Hong Kong (CUHK) is hosting the Advances in Structural Heart Imaging (ASHI) 2026 international forum, reflecting Hong Kong's position as an academic hub in cardiovascular imaging and structural heart disease management. This expertise in advanced imaging is directly relevant to TAVI, where precise pre-procedural planning using cardiac CT and intraprocedural guidance using transoesophageal echocardiography are essential for optimal outcomes.
For GCC patients, Hong Kong's TAVI programme offers several distinct advantages. The city's cardiologists have trained at world-leading institutions and maintain active collaborations with international centres of excellence. The availability of the latest-generation valve platforms ensures that patients have access to the most advanced technology. Additionally, Hong Kong's multilingual healthcare environment, with Arabic interpretation services readily available, ensures clear communication throughout the treatment journey.
Who Is a Candidate for TAVI?
TAVI is indicated for patients with severe symptomatic aortic stenosis. Current guidelines from the European Society of Cardiology (ESC) and the American College of Cardiology/American Heart Association (ACC/AHA) recommend TAVI as the preferred approach for patients aged 75 and older, and as an alternative to surgery for younger patients based on individual risk assessment and patient preference.
The Heart Team approach — a multidisciplinary assessment involving interventional cardiologists, cardiac surgeons, imaging specialists, and anaesthesiologists — is central to the decision-making process. This collaborative evaluation considers the patient's anatomy, comorbidities, frailty status, and personal preferences to determine the optimal treatment strategy.
Patients who are particularly well-suited for TAVI include those with favourable femoral artery access, those who wish to avoid open-heart surgery, patients with significant comorbidities that increase surgical risk, and individuals who prioritise a rapid recovery. Conversely, patients with complex coronary artery disease requiring concurrent bypass surgery, or those with anatomical features unsuitable for transcatheter delivery, may be better served by surgical intervention.
Recovery and Long-Term Outcomes
Recovery following TAVI is remarkably rapid compared with surgical valve replacement. Most patients experience immediate symptom relief, with significant improvements in breathlessness, exercise tolerance, and quality of life within days of the procedure.
A typical recovery timeline includes mobilisation within 6–12 hours, hospital discharge within 1–3 days, return to daily activities within 1–2 weeks, and full recovery within 2–4 weeks. Long-term follow-up data from the landmark trials demonstrate excellent valve durability, with low rates of structural valve deterioration at five to seven years. Ongoing surveillance with annual echocardiography is recommended to monitor valve function.
Conclusion
Transcatheter aortic valve implantation has transformed the treatment of aortic stenosis from a condition requiring major open-heart surgery to one that can be treated through a minimally invasive, catheter-based approach. The accumulation of five-year, six-year, and seven-year follow-up data from randomised controlled trials has confirmed that TAVI delivers outcomes comparable to surgery across the full spectrum of surgical risk. For patients seeking world-class cardiac care, Hong Kong's combination of experienced Heart Teams, advanced imaging capabilities, and access to the latest valve technology makes it an outstanding destination for TAVI.