Transperineal Prostate Biopsy: The Safer, More Accurate Approach to Prostate Cancer Diagnosis
Transperineal prostate biopsy has emerged as the recommended approach for prostate cancer diagnosis, offering near-zero infection rates and superior access to all prostate zones. Dr. Chui Ka Lun, who introduced this technique to Hong Kong, explains the evidence behind this paradigm shift in urological practice.
Introduction
Prostate cancer is the most commonly diagnosed cancer in men worldwide, with over 1.4 million new cases and approximately 375,000 deaths annually [1]. Prostate biopsy remains the definitive diagnostic procedure — it is the only way to confirm the presence of prostate cancer and determine its grade. With more than 3 million prostate biopsies performed globally each year, the choice of biopsy technique has profound implications for patient safety, diagnostic accuracy, and healthcare resource utilisation [2].
For decades, the transrectal ultrasound-guided (TRUS) biopsy was the standard approach: a needle is passed through the rectal wall to sample prostate tissue. While widely practised, this route carries inherent risks — most notably, the passage of the biopsy needle through the bacteria-laden rectum can introduce infection, sometimes leading to life-threatening sepsis. The rising rates of antibiotic-resistant organisms have made this concern increasingly urgent.
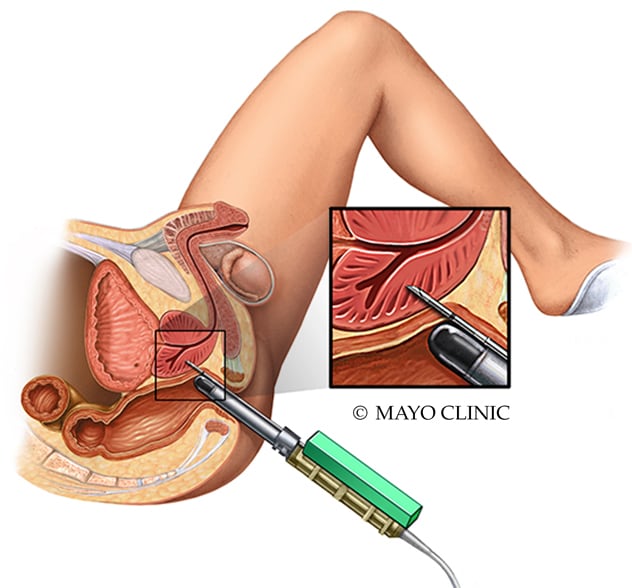
The transperineal (TP) prostate biopsy represents a fundamental paradigm shift. By accessing the prostate through the perineum (the skin between the scrotum and the anus), the needle completely avoids the rectum, virtually eliminating the risk of post-biopsy sepsis. Dr. Chui Ka Lun (崔家倫醫生), a specialist in urology who introduced the transperineal prostate biopsy technique to Hong Kong's urological community, has been at the forefront of this transition, performing over 600 freehand transperineal biopsies under local anaesthesia.
Understanding Prostate Biopsy: Why Is It Necessary?
A prostate biopsy is typically recommended when there is clinical suspicion of prostate cancer, based on one or more of the following findings:
Elevated PSA (Prostate-Specific Antigen): PSA is a protein produced by both normal and malignant prostate cells. While a PSA level above 4.0 ng/mL has traditionally been used as a threshold, the decision to biopsy now incorporates PSA density, PSA velocity, and patient age. The European Association of Urology (EAU) recommends using risk calculators that combine PSA with other clinical variables to determine biopsy necessity [3].
Abnormal Digital Rectal Examination (DRE): A palpable nodule, asymmetry, or induration on DRE raises suspicion for prostate cancer, even in the setting of a normal PSA.
Suspicious Findings on MRI: Multiparametric MRI (mpMRI) has transformed the prostate cancer diagnostic pathway. Lesions scored PI-RADS 3–5 on mpMRI warrant targeted biopsy. The EAU now recommends mpMRI before any prostate biopsy, as it can identify clinically significant cancers while reducing the detection of insignificant ones [3].
Transperineal vs Transrectal: A Head-to-Head Comparison
The landmark PREVENT trial (Prostate Biopsy Randomized Evaluation of Novel Techniques), published in JAMA Oncology in 2024, provided the most definitive evidence comparing the two approaches. This multicentre randomised controlled trial enrolled 742 patients across 38 centres in the United States [2].
Key Findings from the PREVENT Trial
The trial demonstrated that transperineal biopsy achieves equivalent cancer detection while dramatically reducing infectious complications:
| Outcome | Transperineal (n=372) | Transrectal (n=370) | P-value |
|---|---|---|---|
| Clinically significant cancer detection (Gleason ≥2) | 55% | 52% | 0.40 |
| Grade 2+ infection | 0% | 1.6% | 0.02 |
| Urinary retention | 0.3% | 1.1% | 0.20 |
| Bleeding requiring intervention | 0% | 0.3% | — |
The most striking finding was the zero infection rate in the transperineal group, compared to 1.6% in the transrectal group — a statistically significant difference that has accelerated the global shift toward the transperineal approach [2].
Supporting Evidence from Systematic Reviews
Multiple systematic reviews and meta-analyses have corroborated these findings:
Zattoni et al. (2024), in a comprehensive analysis published in European Urology Open Science, confirmed that transperineal and transrectal MRI-fusion biopsies have equivalent diagnostic accuracy for clinically significant prostate cancer [4]. Wu et al. (2024), published in Nature Prostate Cancer, similarly demonstrated equivalent cancer detection rates between the two approaches while highlighting the infection advantage of the transperineal route [5].
A 2025 systematic review and meta-analysis by Mac Curtain et al. in BJUI Compass, encompassing 12 studies and 2,881 patients, specifically examined freehand transperineal biopsy under local anaesthesia. The pooled clinically significant prostate cancer detection rate was 48% overall (52% when combining systematic and targeted biopsies), with a remarkably low complication rate: only 2% experienced Clavien-Dindo grade 1–2 complications, and just 0.1% experienced grade 3–5 complications [6].
The Freehand Technique Under Local Anaesthesia
One of the most significant advances in transperineal biopsy has been the development of the freehand technique under local anaesthesia, which transforms what was traditionally a procedure requiring general anaesthesia and a brachytherapy grid into an outpatient office-based procedure.
How It Works
The freehand technique uses a small-gauge needle guide (such as the PrecisionPoint, CAMProbe, or Tru-Guide system) attached to the transrectal ultrasound probe. The urologist advances the biopsy needle through the perineal skin under real-time ultrasound guidance, without the need for a fixed grid or template.
Step 1 — Preparation: The patient is positioned in the lithotomy position. The perineal skin is cleaned with antiseptic solution. A transrectal ultrasound probe is inserted to visualise the prostate.
Step 2 — Local Anaesthesia: A local anaesthetic (typically 1% lidocaine) is infiltrated into the perineal skin and the periprostatic nerve plexus. The periprostatic block targets the neurovascular bundles at the base of the prostate, providing effective pain control for the sampling phase.
Step 3 — Systematic Sampling: Using the freehand needle guide, the urologist obtains systematic cores from predetermined sectors of the prostate. A typical systematic biopsy involves 12–14 cores distributed across the peripheral zone.
Step 4 — MRI-Targeted Sampling: If mpMRI has identified suspicious lesions (PI-RADS ≥3), additional targeted cores are obtained from these areas using cognitive fusion — the urologist mentally correlates the MRI findings with the real-time ultrasound image to guide the needle to the target.
Step 5 — Completion: The procedure typically takes 15–25 minutes. The patient is observed briefly and can usually return home within 30 minutes.
Pain Tolerance
A common concern about the transperineal approach is whether it is more painful than the transrectal route. The evidence is reassuring. In the Mac Curtain et al. meta-analysis, all studies reported mean or median pain scores below 3 on the Visual Analogue Scale (VAS) or Numerical Rating Scale (NRS), which corresponds to mild pain [6]. The Chiu et al. study from Hong Kong (2020), one of the largest single-centre series with 611 patients, reported a mean VAS pain score of 2.1 ± 1.8, confirming excellent tolerability [7].
Recovery time is also notably shorter compared to template biopsy under general anaesthesia: 18 minutes versus 51 minutes, as reported by Hogan et al. [8].
Why Transperineal Is Safer: The Infection Advantage
The single most compelling argument for the transperineal approach is the dramatic reduction in post-biopsy infection. Understanding why requires an appreciation of the anatomy involved.
The Anatomical Rationale
In transrectal biopsy, the needle traverses the rectal mucosa — a surface colonised by billions of bacteria, including potentially antibiotic-resistant organisms such as fluoroquinolone-resistant Escherichia coli. Despite prophylactic antibiotics, some bacteria inevitably enter the bloodstream or prostatic tissue, leading to infectious complications ranging from urinary tract infections to life-threatening urosepsis.
In transperineal biopsy, the needle enters through the perineal skin — a surface that can be effectively sterilised with standard antiseptic preparation. The rectal wall is never breached, completely eliminating the primary source of bacterial contamination.
Clinical Evidence for Infection Reduction
The evidence supporting the infection advantage of transperineal biopsy is now overwhelming:
The PREVENT trial reported a 0% infection rate in the transperineal group versus 1.6% in the transrectal group (p=0.02) [2]. A systematic review by Basourakos et al. (2022) in European Urology Open Science demonstrated that transperineal biopsy without any antibiotic prophylaxis carries a low risk of sepsis and infection [9]. The ProBE-PC randomised clinical trial by Mian et al. (2024) in The Journal of Urology further confirmed significantly fewer infectious complications with the transperineal approach [10].
This evidence has led multiple international guidelines to recommend the transperineal approach:
| Guideline Body | Recommendation |
|---|---|
| European Association of Urology (EAU) 2024 | Strongly recommends transperineal approach [3] |
| National Institute for Health and Care Excellence (NICE) | Recommends transperineal approach |
| American Urological Association (AUA/SUO) | Recommends either route; acknowledges TP advantages for infection |
Superior Anatomical Access
Beyond infection safety, the transperineal approach offers inherent anatomical advantages for prostate sampling.
Anterior Zone Access
The anterior prostate — the region furthest from the rectum — is notoriously difficult to sample via the transrectal route. Anterior tumours account for approximately 20–30% of prostate cancers and are frequently missed by transrectal biopsy. The transperineal approach provides a direct trajectory to the anterior gland, improving the detection of these cancers [11].
Apical Zone Sampling
The prostatic apex, located at the most inferior aspect of the gland near the external urethral sphincter, is another region where transperineal access is superior. Adequate sampling of the apex is critical because apical tumours can be aggressive and their detection influences surgical planning.
Sectoral Analysis
The Hong Kong study by Chiu et al. (2020) provided detailed sectoral analysis of cancer detection by transperineal biopsy, demonstrating consistent sampling across all prostate zones — anterior, posterior, lateral, medial, base, mid-gland, and apex — confirming the comprehensive coverage achievable with this technique [7].
The Role of MRI in Modern Prostate Biopsy
Multiparametric MRI (mpMRI) has become an integral component of the prostate cancer diagnostic pathway. The EAU guidelines now recommend mpMRI before any prostate biopsy [3].
The MRI-Targeted Biopsy Pathway
The modern diagnostic pathway typically follows these steps:
- Clinical suspicion (elevated PSA, abnormal DRE, family history)
- mpMRI of the prostate — scored using PI-RADS v2.1
- Risk stratification — PI-RADS 1–2 (low suspicion) may avoid biopsy; PI-RADS 3–5 warrants biopsy
- Combined systematic + targeted biopsy — the EAU recommends performing both systematic and MRI-targeted biopsies to maximise detection of clinically significant cancer [3]
Cognitive Fusion vs Software Fusion
MRI-targeted biopsies can be performed using either cognitive fusion (the urologist mentally correlates MRI and ultrasound images) or software-assisted MRI/US fusion. A comprehensive review has demonstrated that when combined with systematic biopsy, the results between cognitive fusion and software-targeted approaches are similar, with cognitive fusion being more accessible and cost-effective [12].
Who Should Consider Transperineal Prostate Biopsy?
Transperineal prostate biopsy is appropriate for all men who require a prostate biopsy. It is particularly advantageous in the following scenarios:
First-time biopsy: For men undergoing their initial prostate biopsy, the transperineal approach provides comprehensive sampling with minimal infection risk, making it the ideal first-line approach.
Repeat biopsy after negative TRUS biopsy: Men with persistently elevated PSA or suspicious MRI findings despite a previous negative transrectal biopsy benefit from the transperineal approach, which can access anterior zones that may have been under-sampled.
Patients on anticoagulation therapy: The transperineal approach allows for effective haemostasis through perineal compression, making it safer for patients who cannot discontinue blood-thinning medications.
Patients with rectal pathology: Men with inflammatory bowel disease, rectal surgery, or other anorectal conditions may be unable to undergo transrectal biopsy, making the transperineal route the only option.
Active surveillance monitoring: For men on active surveillance for low-grade prostate cancer, serial transperineal biopsies provide consistent, comprehensive sampling to monitor for disease progression.
Dr. Chui Ka Lun: Pioneering Transperineal Biopsy in Hong Kong
Dr. Chui Ka Lun (崔家倫醫生) is a specialist in urology holding qualifications of MBBS (HKU), FRCSEd, FCSHK, FRCSEd(Urol), and FHKAM (Surgery). He is recognised as a pioneer who introduced three advanced surgical procedures to Hong Kong's urological community: Holmium Laser Enucleation of the Prostate (HoLEP), transperineal prostate biopsy, and transurethral seminal vesiculoscopy.
Dr. Chui's extensive experience with the freehand transperineal technique under local anaesthesia has contributed to a substantial body of clinical data demonstrating the safety and efficacy of this approach in the Hong Kong population. His work aligns with the landmark Chiu et al. (2020) study — one of the largest single-centre series globally with 611 patients — which demonstrated excellent cancer detection rates and tolerability for freehand transperineal biopsy under local anaesthesia [7].
Beyond his clinical practice, Dr. Chui is deeply committed to community service and medical advancement. He has championed the charitable joint replacement programme "Walk With You, Stand Up" (與你同行站起來) through the HKFTU Specialist Clinic. He has also led delegations of Hong Kong doctors to visit hospitals in mainland China, promoting cross-border medical collaboration within the Greater Bay Area (GBA) and encouraging Hong Kong physicians to explore multi-site practice opportunities across the region.
What to Expect: Before, During, and After the Procedure
Before the Biopsy
Your urologist will review your PSA history, DRE findings, and MRI results. You will be advised about medication adjustments — most blood-thinning medications can be continued for transperineal biopsy, though this should be discussed individually. Unlike transrectal biopsy, no bowel preparation or rectal enema is required, and in many protocols, no prophylactic antibiotics are needed [9].
During the Procedure
The procedure is performed as an outpatient under local anaesthesia. You will be positioned on your back with your legs supported. After perineal skin preparation and local anaesthetic injection, the urologist will obtain biopsy cores under ultrasound guidance. Most patients describe the sensation as mild pressure or brief discomfort. The entire procedure typically takes 15–25 minutes.
After the Procedure
You will be observed for approximately 30 minutes before discharge. Common post-procedure experiences include:
- Blood in urine (haematuria): Mild blood-tinged urine is normal and typically resolves within 3–5 days
- Blood in semen (haematospermia): May persist for several weeks and is harmless
- Perineal bruising: Mild bruising at the needle entry site is common and resolves spontaneously
- Urinary discomfort: Mild burning or frequency may occur for 1–2 days
Serious complications are extremely rare. The pooled rate of significant complications (Clavien-Dindo grade 3–5) across 2,881 patients in the Mac Curtain et al. meta-analysis was only 0.1% [6].
Recovery Timeline
| Timeframe | Expected Recovery |
|---|---|
| Day 0 | Procedure completed; return home same day |
| Days 1–3 | Mild urinary symptoms; blood-tinged urine |
| Days 3–7 | Most symptoms resolve; resume normal activities |
| Week 2 | Biopsy results typically available |
| Weeks 2–6 | Haematospermia may persist (harmless) |
Frequently Asked Questions
Q: Is transperineal biopsy more painful than transrectal biopsy? A: Studies show that pain levels are comparable between the two approaches when adequate local anaesthesia is used. Most patients report only mild discomfort (pain score 2–3 out of 10). The transperineal approach avoids the discomfort of rectal probe manipulation that some patients find distressing.
Q: Do I need to stop my blood-thinning medications? A: In many cases, anticoagulation therapy can be continued for transperineal biopsy, as perineal compression provides effective haemostasis. However, this should be discussed with your urologist on an individual basis.
Q: How many tissue samples are taken? A: A standard systematic biopsy involves 12–14 cores. If MRI has identified suspicious areas, an additional 2–4 targeted cores are taken from each lesion, bringing the total to approximately 14–22 cores.
Q: Will I need antibiotics? A: Many centres now perform transperineal biopsies without prophylactic antibiotics, as the infection risk is extremely low. Your urologist will advise based on their institutional protocol.
Q: How soon will I get my results? A: Biopsy results are typically available within 7–14 days. Your urologist will schedule a follow-up appointment to discuss the findings and any recommended next steps.
Q: Can the biopsy miss a cancer? A: No biopsy technique can guarantee 100% detection. However, combining systematic sampling with MRI-targeted biopsies significantly improves the detection of clinically significant cancers while reducing the detection of insignificant ones.
Why Choose Hong Kong for Transperineal Prostate Biopsy?
Hong Kong offers a unique combination of advantages for international patients seeking prostate biopsy:
- World-class medical infrastructure with JCI-accredited hospitals and state-of-the-art imaging facilities
- Experienced urologists trained in the latest transperineal techniques, with extensive case volumes
- Bilingual medical staff proficient in English and Chinese, with Arabic interpretation services available
- Visa-free entry for GCC nationals (UAE, Saudi Arabia, Qatar, Kuwait, Bahrain, Oman)
- Muslim-friendly environment with halal dining options, prayer facilities, and culturally sensitive care
- Direct flights from major Gulf cities (Dubai, Abu Dhabi, Riyadh, Doha, Kuwait City)
- Rapid turnaround — consultation, MRI, and biopsy can often be completed within a single visit
References
- Culp MB, et al. Recent global patterns in prostate cancer incidence and mortality rates. Eur Urol. 2020;77(1):38–52.
- Hu JC, et al. Transperineal vs transrectal prostate biopsy — the PREVENT randomized clinical trial. JAMA Oncol. 2024;10(11):1590–1593.
- European Association of Urology. EAU Guidelines on Prostate Cancer. 2024.
- Zattoni F, et al. Transperineal vs transrectal MRI-fusion prostate biopsy: diagnostic accuracy comparison. Eur Urol Open Sci. 2024.
- Wu RC, et al. Transperineal vs transrectal prostate biopsy: cancer detection and complications. Nat Prostate Cancer. 2024.
- Mac Curtain BM, et al. Transperineal prostate biopsy with freehand technique under local anaesthetic: a systematic review and meta-analysis. BJUI Compass. 2025;6(4):e70016.
- Chiu PK, et al. Sectoral cancer detection and tolerability of freehand transperineal prostate biopsy under local anaesthesia. Prostate Cancer Prostatic Dis. 2021;24(2):431–438.
- Hogan D, et al. Local versus general anesthesia transperineal prostate biopsy: tolerability, cancer detection, and complications. BJUI Compass. 2021;2(6):428–435.
- Basourakos SP, et al. Role of prophylactic antibiotics in transperineal prostate biopsy: a systematic review and meta-analysis. Eur Urol Open Sci. 2022;37:53–63.
- Mian BM, et al. Complications following transrectal and transperineal prostate biopsy: results of the ProBE-PC randomized clinical trial. J Urol. 2024;211(2):205–213.
- Uleri A, et al. Impact of transperineal versus transrectal MRI-targeted biopsy on clinically significant prostate cancer detection rate. Eur Urol Oncol. 2023;6(6):621–628.
- Kanagarajah A, et al. A systematic review on the outcomes of local anaesthetic transperineal prostate biopsy. BJU Int. 2023;131(4):408–423.